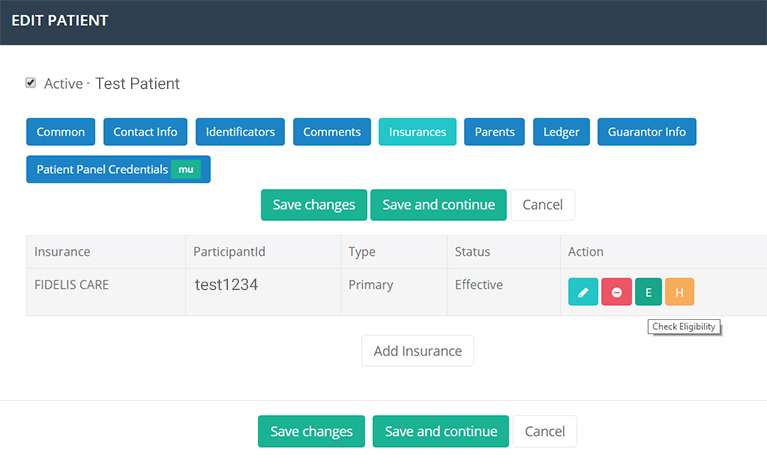
It is very important for any provider to check patient' insurance eligibility before rendering medical services. The patient's eligibility is usually verified at the front desk by medical staff. This helps to save time for doctors and increase revenue at time of service.
Patients, both established and new, should have their insurance cards in any medical setting. The medical staff checks if the information on the card is relevant to the date of visit. It can be done by several ways – by phoning to insurance representative or checking on the insurance website. If the front desk staff faces any problems, the patient has to pay for the service or arrange payment by another way.
Billing companies confirm that claims are denied and have to be appealed due to the various reasons where eligibility-related delays are not on the last place. It influences providers' income which consists of doctor skills and knowledge. However, such “late” claims are not always paid.
So, patient insurance eligibility is the first and essential step to get full reimbursement that a doctor really deserves. That function is implemented in iSmart EHR system and always up-to-date for any patient and provider.
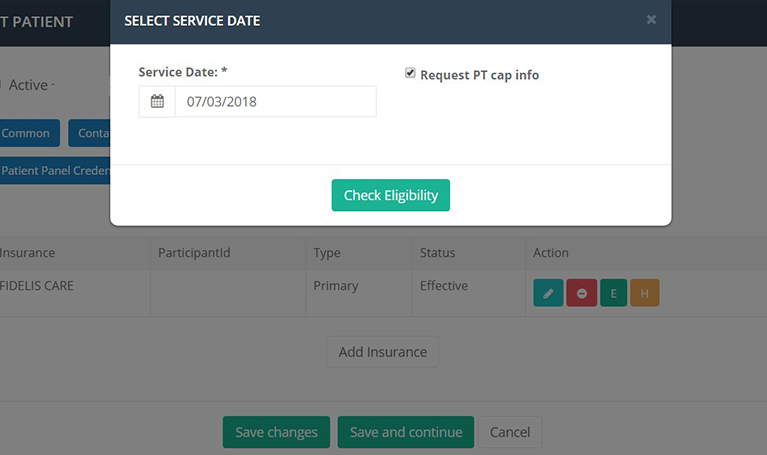
NEWS! As of May 2018 users can request physical therapy cap information within the eligibility request. Newly enrolled users with iSmart Package A subscription may have up to 100 free eligibility requests for the first 3 months.
Have practice that need eligibility functionality only? There is a stand-alone solution that allows requesting more than 700 payers. Eligibility of WCH - no extra actions and very easy setup.
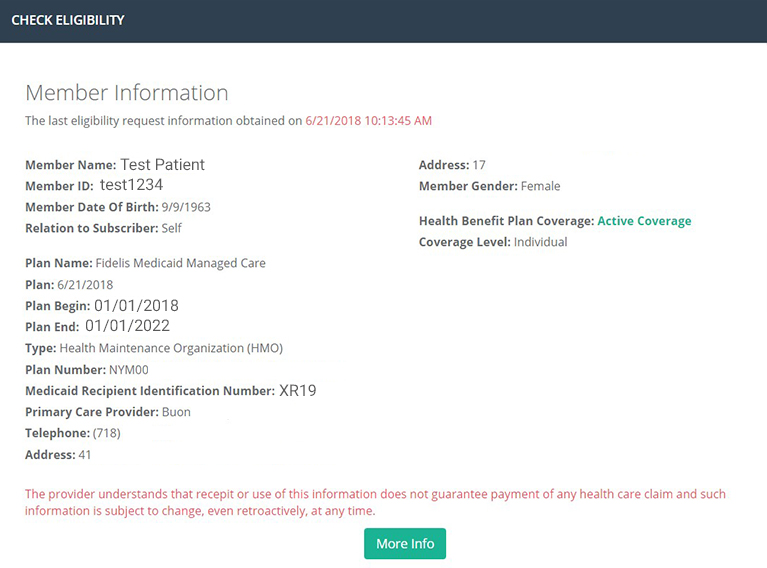
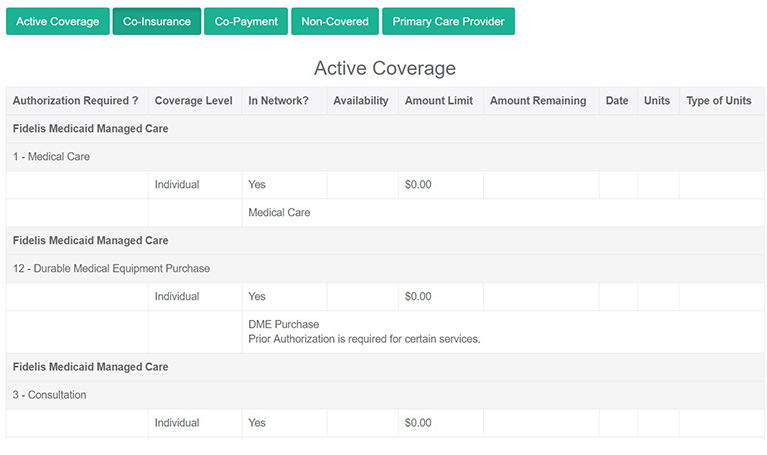
Click one button in the patient information section of WCH’s iSmart EHR to access any payer’s eligibility summary. An additional link leads to more detailed information on a patient’s copay, deductible, covered services, and more.